During National Hospital Week, the Texas Hospital Association is proud to celebrate the hospitals, health systems and care teams working every day to improve the health and well-being of Texans. From expanding access to specialty and preventive care to responding during natural disasters and delivering life-saving transplants, Texas hospitals serve as essential pillars of their communities.
Across every region of the state, physicians, nurses, clinicians and support staff are advancing innovative care, strengthening access for underserved populations and providing compassionate treatment during some of life’s most critical moments. The following stories highlight just a few of the many ways Texas hospitals are transforming care and saving lives every day.
DHR Health: Providing Critical Access to Care in the Rio Grande Valley
DHR Health is helping expand access to life-saving specialty care in the Rio Grande Valley through its Transplant Institute, which reached a major milestone in 2025 with 101 kidney transplants completed since the program’s founding in 2017.
Each transplant represents a patient transitioning from life on dialysis to renewed health and independence, reflecting the profound clinical and personal impact of advanced kidney care in a region with high rates of chronic disease. Conditions such as diabetes, hypertension and obesity are particularly prevalent in the Rio Grande Valley and significantly increase the risk of kidney failure, contributing to sustained demand for transplant services. With approximately 4,000 patients currently on dialysis in the region, timely access to transplant care remains a critical need.

DHR Health’s multidisciplinary transplant team provides comprehensive support across the full continuum of care, including patient evaluation, surgical intervention and long-term post-transplant management. This coordinated approach ensures that patients receive consistent, specialized care close to home, improving both access and continuity of treatment.
As the only transplant center of its kind south of San Antonio and Houston, DHR Health plays a unique role in reducing geographic and financial barriers that often require patients to travel long distances for advanced care. By keeping these services local, the health system helps alleviate strain on families while strengthening regional healthcare capacity.
The 101-transplant milestone underscores DHR Health’s broader commitment to addressing critical gaps in specialty care across underserved communities. Through sustained investment in clinical expertise and infrastructure, the organization continues to expand access to world-class care while improving outcomes for patients across South Texas.
Peterson Health: Providing Critical Trauma Care Amid Hill Country Flood Response
When catastrophic flooding struck Kerrville over the July 4 holiday, Peterson Health quickly shifted from routine operations to full disaster response – serving as a critical access point for injured residents across the region. Activating established emergency protocols, the hospital prepared for a surge of patients while its emergency department rapidly triaged those arriving with flood-related injuries.

Inside the hospital, care teams worked in tight coordination to stabilize and treat patients presenting with fractures, lacerations, crush injuries and complications from contaminated floodwaters. As the volume and acuity of cases increased, surgical teams pivoted in real time – transitioning operating rooms from scheduled procedures to urgent trauma care. In some cases, patients arrived in critical condition, requiring immediate intervention to address life-threatening injuries sustained in fast-moving water and debris.
This seamless coordination between emergency, surgical and inpatient teams underscores the hospital’s ability to function in a mass-casualty environment, despite the challenges of serving a rural community with limited regional resources. Clinicians moved patients efficiently through triage, imaging, surgery and recovery, ensuring timely, lifesaving care during the most critical window.
While the hospital’s primary focus remained on stabilizing and treating incoming patients, Peterson Health’s response extended beyond its walls. Staff supported first responders and community recovery efforts, reflecting the broader role hospitals play during disasters – not only as centers for acute care, but as anchors of community resilience.
In the aftermath of the floods, Peterson Health’s trauma response highlights the essential role of prepared, coordinated hospital teams in delivering care when communities need it most.
Clarity Child Guidance Center: Expanding Trauma Informed Mental Health Care to Youth
For many children receiving mental health treatment, trauma is not a single moment but a lasting experience that shapes how they respond to care, trust providers and navigate daily life. At Clarity Child Guidance Center, where an estimate of nearly 90% of patients served have experienced some form of trauma, that reality has guided the organization’s approach to treatment for more than a decade.
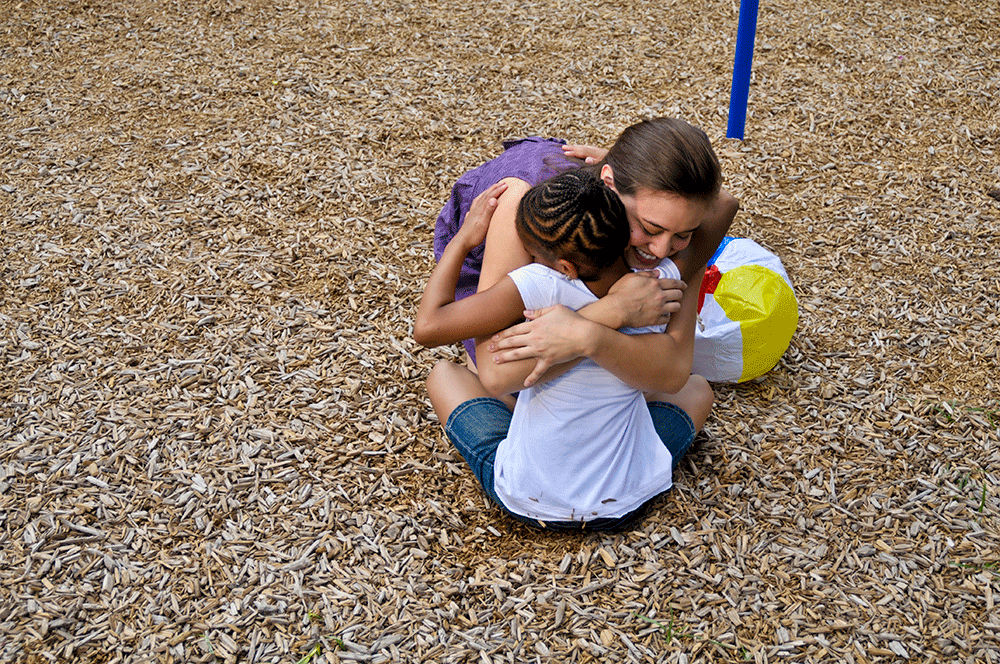
In May 2025, Clarity earned the Level 1 Foundational Trauma-Informed Care Organizational Certification from The Ecumenical Center, recognizing the organization’s commitment to creating environments centered on safety, trust, collaboration and empowerment for both patients and staff.
The certification followed a two-year process that included staff education, organizational assessments, participant feedback and a site visit evaluating how trauma-informed principles are integrated throughout the facility. While Clarity’s clinical teams have long used trauma-informed treatment practices, the certification expanded those principles across all departments, including employee engagement, communication and family collaboration.
According to Clarity leadership, the process also strengthened transparency with patients and families by increasing opportunities for feedback and improving communication around treatment expectations and goals.
“Trauma informed care is a perfect fit for the treatment approach that we use at Clarity Child Guidance Center,” Clarity CEO and President Jessica Knudsen, LCSW, FACHE, says. “The certification process was a great reminder that we need to utilize the same level of empathy with our peers and colleagues as we do with our families in need of services.”
As mental health needs among children and adolescents continue to grow, Clarity’s certification reflects a broader commitment to building systems of care that recognize the long-term impact of trauma while creating supportive environments where children and families can begin to heal.
Texas Children’s Hospital: Transforming Pediatric Heart Care Through Transplant Innovation
At Texas Children’s Hospital, three young boys facing end-stage heart failure became connected in an unexpected way as they each underwent life-saving heart transplants just days apart.

Each child was treated within the hospital’s nationally recognized pediatric heart transplant program, where complex cardiac cases require constant coordination between pediatric cardiologists, transplant surgeons, intensivists, anesthesiologists and transplant coordinators. Prior to surgery, all three patients required intensive stabilization and advanced life-support measures, including continuous monitoring and mechanical support, as they waited for suitable donor hearts.
When organs became available, Texas Children’s teams moved quickly to align surgical timing, operating room readiness and post-transplant care plans. Each transplant required precise coordination across multiple specialties to ensure the best possible outcome for some of the hospital’s most medically fragile patients. Texas Children’s is one of the nation’s leading pediatric transplant centers, with extensive experience managing high-acuity cases and delivering outcomes shaped by decades of specialized expertise.
Beyond the clinical complexity, the children’s shared experience also became a source of connection. While undergoing treatment in adjacent units, the boys formed a bond – offering encouragement and companionship to one another and their families during an emotionally intense and uncertain time.
Following successful surgeries, each child transitioned into recovery and rehabilitation, beginning the long-term process of healing that includes medication management, cardiac monitoring and ongoing follow-up care.
Their intertwined journeys reflect the depth of pediatric specialty care at Texas Children’s – where advanced medicine, multidisciplinary teamwork and human connection come together to give children facing the most critical diagnoses a renewed chance at life.
United Regional Health Care System: Expanding Access to Preventive Care Through Community-Based Health and Nutrition Services
United Regional Health Care System is addressing the intersecting challenges of food insecurity and chronic disease in Wichita Falls through an innovative partnership with the Wichita Falls Area Food Bank. Together, they launched the Mobile Pantry Health Screenings Program, bringing preventive care and nutrition support directly into communities facing some of the region’s most significant health disparities.
Originally launched in 2019 and expanded in subsequent years, the program integrates affordable, nutritious food access with on-site health services at mobile pantry locations. Each event includes free screenings such as blood pressure and blood glucose checks, influenza vaccinations and personalized health education. A registered nurse and patient advocate from United Regional also provide care navigation, connecting individuals to primary care providers, medications and additional social services based on identified needs.
The program was developed in response to United Regional’s 2022 Community Health Needs Assessment, which identified food insecurity, limited primary care access and high rates of chronic conditions – particularly diabetes and heart disease – as leading health concerns in Wichita County. By embedding clinical support within existing food distribution efforts, the initiative reduces barriers to care while meeting residents where they already seek essential resources.
Between 2022 and 2024, the program reached more than 31,000 households and identified over 2,500 individuals with elevated blood pressure or blood glucose levels. Many of these patients have since been connected to ongoing care, including chronic disease management, primary care access and social support services.
By combining nutrition access with preventive health interventions, United Regional’s Mobile Pantry Health Screenings Program is strengthening early detection, improving care linkage, and advancing long-term community health across Wichita Falls and Wichita County.
Related articles from The Scope
Now Boarding: THA’s Newest Board of Trustees Members
The Texas Hospital Association’s Board of Trustees plays a critical…
Cris Daskevich: People-First Leadership
Long before she led in hospital hallways, Cris Daskevich’s instincts…
New Year, New Momentum: THA’s 2026 Focus
3… 2… 1… Happy New Year from THA! As we…
THA’s Holiday Tribute to the Heroic Work of Texas Hospitals
This holiday season, we celebrate the extraordinary expertise, compassion and…
2025 Newsmakers in Texas Hospitals
Sponsored by Envision Healthcare, THA’s Newsmakers are hospital executives and…
Leading Texas Hospitals: Honoring Service Beyond the Uniform This Veterans Day
This Veterans Day, THA is proud to honor four veterans…






