This article is sponsored by the Anesthesia Remediation & Reentry Program. This article does not necessarily speak to or reflect policy positions of THA.
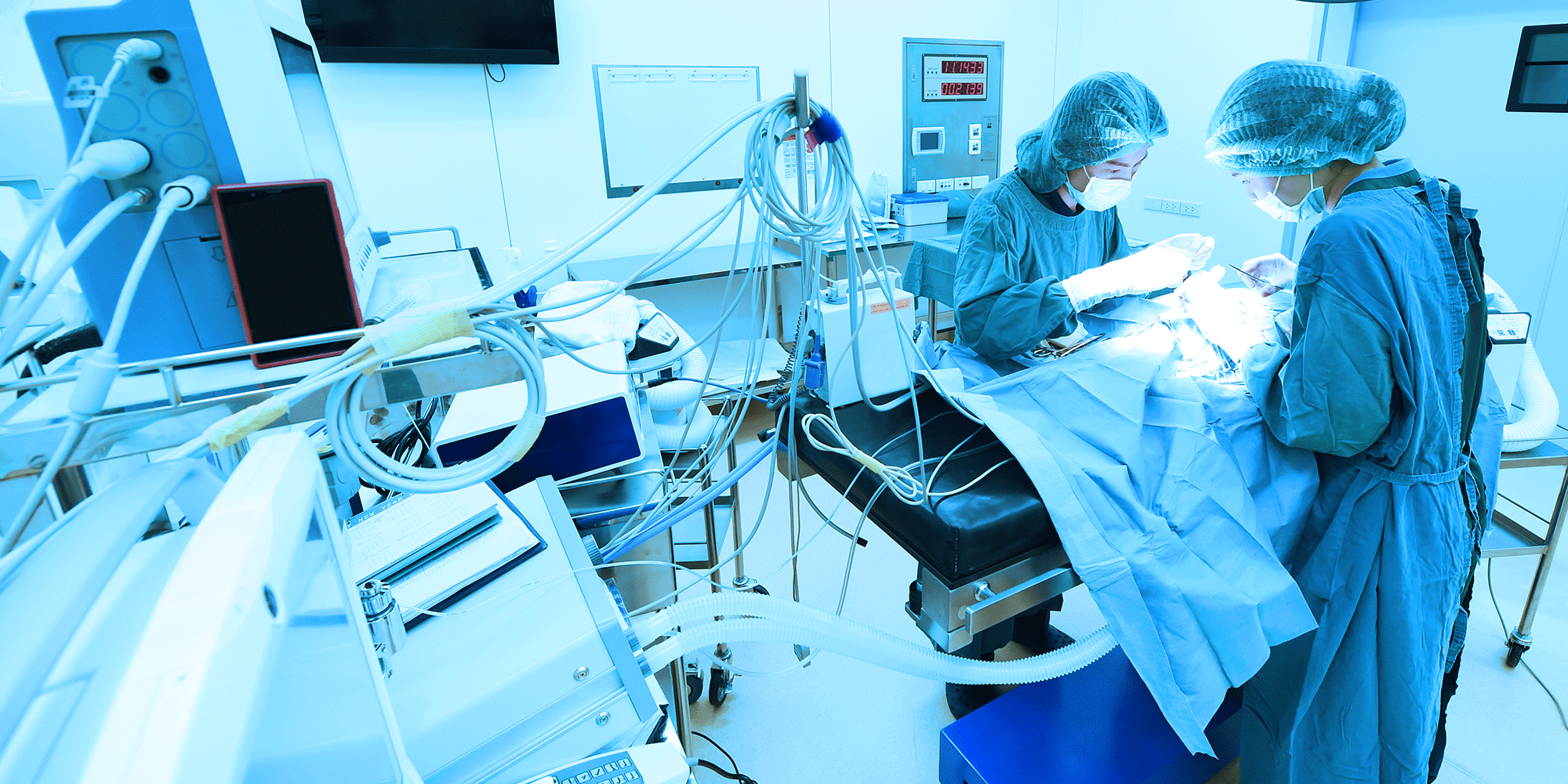
The signs are everywhere. A surgeon’s elective caseload quietly shrinks; profitable service line stalls, and patients are repeatedly rescheduled. For a growing number of Texas hospitals, this is not a theoretical risk. It is the daily reality of a fragile anesthesia workforce contracting faster than the pipeline can replenish it.

The numbers underscore how serious the situation has become. The Health Resources and Services Administration (HRSA) projects a national shortage of roughly 8,450 anesthesiologists by 2037,1 and a separate workforce analysis puts the gap at 6,300 physicians by 2036.2 Meanwhile, about 57 percent of practicing anesthesiologists are over the age of 55, with more than 17 percent nearing retirement.3 The CRNA pipeline faces comparable pressure: the AANA reports that 12 percent of CRNAs plan to retire by 2027.4
Training capacity is not absorbing the shock. In the 2025 Match, more than 3,000 students applied for 1,805 anesthesiology residency positions – leaving roughly 40 percent of applicants unmatched.5 Expanding residency programs takes a minimum of two years and substantial investment, and retirements are accelerating faster than new graduates arrive. In 2023, 78 percent of health care facilities reported an anesthesia staffing shortage – more than double the pre-pandemic figure of 35 percent.6 Locum tenens coverage can bridge an immediate gap, but at a cost that is rarely sustainable.
What is rarely discussed in workforce planning is that a meaningful supply of fully-trained anesthesiologists already exists – they are simply not practicing or not practicing at full scope. Some have moved to outpatient and procedure center settings (e.g. cataract, pain and endoscopy centers). Some stepped away from clinical work entirely for family, health, or administrative reasons. Others hold board certification but have gaps in current skills or hospital credentialing requirements. This cohort of clinicians are trained physicians whose knowledge and skills have narrowed or lapsed – and who, with the right structured support, are ready to return.
Since 2021, the Anesthesiology Remediation and Refresher Program (ARRP), described in the August 2022 edition of ASA Monitor7, ARRP (http://www.arrp.us) partners with hospitals nationwide to implement structured, on-site programs tailored to the expectations and needs of their respective anesthesia departments.
The program serves four cohorts: physicians returning from narrow-scope settings, clinicians who took extended time away, anesthesiologists with complex supervisory or regulatory requirements, and those with board certification gaps. All completed residency but require more than updating a CV to regain hospital privileges.
ARRP uses a four-phase progression: observation, assistance, close direction, and general supervision – with each phase calibrated to the individual’s baseline and gaps. Remediation covers clinical skills, regional techniques, monitoring, documentation, and compliance. Most programs run for about a year, though timelines vary. Critically, enrollees contribute to OR throughput under supervised practice from early stages.
For hospitals, the program’s value is immediate and compounding. Enrollees strengthen the resilience of an anesthesia department during the program itself. Upon graduation, many remain at the affiliate institutions, reducing recruitment costs and adding a credentialed clinician to the permanent roster. The program’s structure is designed to satisfy bylaws and other governance requirements, making the pathway through medical staff privileging more predictable than ad hoc reentry attempts. Affiliate hospitals pay a startup and maintenance fee to ARRP; enrollees pay a program fee upon completion.
Governance matters as much as clinical rigor. Traditional credentialing processes are not designed for physicians returning after years out of practice. ARRP documents supervision, case logs, and performance milestones – providing committees with the evidence needed to approve physician reentry confidently.
Texas hospitals are not short on ambition or operational capability. What many are short on is a practical mechanism for rebuilding anesthesia workforce depth without waiting on the residency pipeline to catch up – a wait measured in years, not months. Remediation and reentry programs will not replace the need for training expansion or retention strategies. But for health systems willing to work in true partnership with their existing anesthesia leadership, they offer something locums’ coverage does not: the beginning of a sustainable talent pipeline, built within your own walls.
ABOUT Anesthesia Remediation & Reentry Program (ARRP)
ARRP partners with hospitals and anesthesia groups to implement structured, hospital-based programs that safely reintegrate qualified, board-trained anesthesiologists into full clinical practice.
Contact us at [email protected] | 727-355-266
FOOTNOTES
- Health Resources & Services Administration (HRSA). National and Regional Supply and Demand Projections for the Nurse Anesthetist, Nurse-Midwife, and Nurse Practitioner Workforces: 2020–2035. U.S. Department of Health and Human Services; 2022. HRSA projects a shortage of approximately 8,450 anesthesiologists by 2037 under base-case assumptions.
- Medicus Healthcare Solutions. The Anesthesia Provider Shortage White Paper. 2025. Available at: medicushcs.com. Report projects a shortage of 6,300 anesthesiologists by 2036.
- Medicus Healthcare Solutions. The Anesthesia Provider Shortage: Confronting the Growing Demands for Care. 2025. In 2020, the average age of practicing anesthesiologists was 52.6; 56.9% were older than 55, with more than 17% nearing retirement.
- American Association of Nurse Anesthesiology (AANA). CRNA workforce survey data cited in: Medicus Healthcare Solutions. The Anesthesia Provider Shortage: Confronting the Growing Demands for Care. 2025. AANA reports 12% of CRNAs plan to retire by 2027.
- National Resident Matching Program (NRMP). 2025 Main Residency Match Results and Data. Washington, DC: NRMP; 2025. Of 3,000+ anesthesiology applicants, 1,805 PGY-1 positions were offered; approximately 40% of applicants went unmatched.
- Abouleish AE, et al. The Anesthesia Workforce: Supply and Demand. Anesthesiology. June 2024. By 2023, 78% of facilities reported an anesthesia staffing shortage, compared with 35% before the COVID-19 pandemic.
- Gallagher A. Exploring NUMC’s Anesthesia Remediation and Refresher Program. ASA Monitor. 2022;86(8):37. doi: 10.1097/01.ASM.0000855704.28944.46. Nassau University Medical Center’s ARRP program was described in the American Society of Anesthesiologists’ member journal as an innovative model for reintegrating anesthesiologists into hospital practice.
Related articles from The Scope
The Evolution of Patient Discharge Carts
Why should your hospital use CarryAll patient discharge carts? Because…
Streamlining Patient Discharges: How RAPTR Saves Time & Money
Acadian Ambulance Service is proud to launch a new integrated…
Rethinking the Hospital Workforce: Beyond Staffing, Toward Strategy
Hospitals across Texas and beyond are navigating one of the…
Mergers, Medicaid & the Math Behind Rural Hospital Endurance
Declining reimbursements, workforce shortages, and policy shifts have caused many…
Turning Coverage Gaps into Sustainable Solutions
Hospitals across the state know the story: a physician leaves,…
The Nursing Shortage is a Solvable Problem — If We Rethink the Pipeline
At first glance, the nursing shortage looks like it may…